COVID-19, a disease caused by the new SARS-CoV-2 coronavirus, which is widely known to cause a severe acute respiratory syndrome, believed to be the death of patients infected with the pathogen, is more complex than previously understood, and not only attacks the pulmonary system, it can affect the human being – literally – from the brain to the toes.
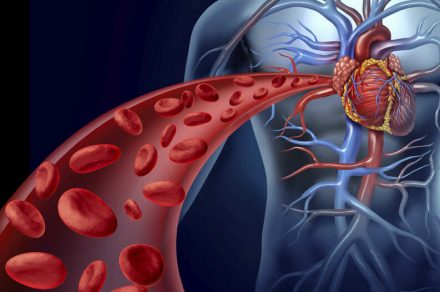
The new coronavirus can spread in humans and kill its victims in different ways. Numerous doctors and scientists agree that COVID-19 not only damages the lungs, but also spreads to other organs such as the heart, blood vessels, kidneys, intestines, and the brain.
This is reviewed in an article published last Friday, April 17 in the journal Science, which explains how COVID-19 even attacks cells in the human body.
«It can attack almost anything in the body, with devastating consequences», said Harlan Krumholz, a cardiologist at Yale University in the United States, adding that «its ferocity is impressive and humiliating».
The study indicates that a COVID-19 infection begins when SARS-CoV-2 enters the nose and / or throat of a person who has inhaled drops expelled into the air by another person infected with the virus.
The cells of the lining of the nose are rich in a receptor called angiotensin-that converts the enzyme 2 (ACE2), to which COVID-19 binds to so as to enter the cell. Once inside, the virus hijacks the cell’s machinery, making countless copies of itself to invade new cells.
As the virus multiplies, an infected person may have no symptoms or instead, develop fever, dry cough, sore throat, loss of smell and taste, or headaches and body aches. If the immune system does not counteract the virus during this initial phase, the infection goes down the trachea to attack the lungs, where it can become fatal.
The body’s battle with the virus disrupts the healthy transfer of oxygen. Thus, first-line white blood cells release inflammatory molecules, called chemokines, which in turn summon more immune cells that attack and kill virus-infected cells, leaving behind fluid and dead cells.
This is the underlying pathology of pneumonia, with its corresponding symptoms: cough, fever, and rapid, shallow breathing. While some patients recover with the support of inhaled oxygen through the nostrils, others develop acute respiratory distress syndrome and end up requiring pulmonary ventilators.
Some scientists suspect that the severity of certain cases is due to a reaction of the immune system, known as a ‘cytokine storm’, which occurs when immune cells begin to attack healthy tissues. The thing is that COVID-19 seems to be able to attack other organs of the human body as well.

COVID-19 attacks blood vessels and the heart
Dozens of studies indicate that the virus also attacks the heart and blood vessels. An investigation showed heart damage in nearly 20% of 416 COVID-19 patients in the Chinese city of Wuhan. Another study states that 44% of 36 patients admitted to intensive care in Wuhan had arrhythmias.
Furthermore, the virus appears to spread to the blood as well. Among the 184 patients admitted to intensive care with COVID-19 in the Netherlands, 38% of them had abnormally coagulating blood, while almost a third already had clots, which can separate and reach the lungs to block vital arteries, one condition known as pulmonary embolism. Blood clots in the arteries can also lodge in the brain and cause a stroke.
The infection can also lead to constriction of the blood vessels. There are reports of ischemia in the fingers and toes, a reduction in blood flow that can lead to swelling, finger pain, and tissue death.
Also, at some stages of the disease, the virus may upset the balance of hormones that help regulate blood pressure and constrict the blood vessels to the lungs.
According to another study, 27% of 85 hospitalized patients in Wuhan experienced kidney failure. Other research found that 59% of nearly 200 patients hospitalized for COVID-19 in the Chinese provinces of Hubei and Sichuan had protein in the urine, and another 44% had blood in the urine, suggesting damage of the kidney.
People with acute kidney damage prior to a COVID-19 infection were five times more likely to die than those without kidney disease, the same investigation concluded.
Cytokine storms can also dramatically reduce blood flow to the kidneys, causing fatal damage.

Damage to the brain and intestines
Other doctors suggest that the new coronavirus may also attack the brain and central nervous system. These specialists have treated patients who were infected with COVID-19 and at the same time suffered from inflammatory brain encephalitis or seizures.
Some of these people, when infected by SARS-CoV-2, lost consciousness briefly, while others suffered strokes or lost their sense of smell.
A recent study reported certain traces of the new coronavirus in the cerebrospinal fluid of a COVID-19 patient who developed meningitis and encephalitis.
However, keep in mind that there are other factors that may be damaging the brain. For example, a cytokine storm could cause brain inflammation, and an exaggerated tendency for blood to clot could trigger strokes.
The disease can also infect the lining of the lower digestive tract. A Chinese team reported finding the protein coat of the virus in gastric, duodenal, and rectal cells in biopsies from a COVID-19 patient.
The intestines are not the last destination for the disease to pass through the body. For example, some hospitalized patients developed conjunctivitis, although it is not clear if the virus directly invades the eye.
Meanwhile, other reports suggest liver damage: More than half of the COVID-19 patients hospitalized at two Chinese centers had elevated levels of enzymes indicating injury to the liver or bile ducts.

Attacks of the COVID-19 on the blood system
The conclusions of the first autopsies of people who died from COVID-19, carried out at the Polyclinic Hospital in Milan, Italy, were directed at the lungs, according to the evidence provided in advance by cardiologist Miguel Ángel García Fernández and published in the Redacción Médica journal.
The BMJ magazine collects a publication that expands the information, focused on lung damage, based on these first autopsies. In the study published in BMJ, the experts point out that “the characteristics of the exudative and proliferative phases of diffuse alveolar disease (DAD) were found: capillary congestion, pneumocyte necrosis, hyaline membrane, interstitial edema, pneumocyte hyperplasia and reactive atypia, and platelet fibrin thrombi».
The main relevant finding, according to the publication, “is the presence of platelet fibrin thrombi in small arterial vessels. This important observation adjusts to the clinical context of coagulopathy that dominates in these patients and is one of the main goals of therapy».
The investigation of the lung tissue was carried out in a total of 38 patients who died after an average time of 16 to 27 days from the onset of the symptoms of the disease.
«Macroscopic examination of the lungs revealed heavy, congested and edematous organs with irregular involvement», explained the researchers. As for the ultrastructural examination, this «revealed viral particles, with a typical morphology of the Coronaviridae family and located along the plasmalemal membranes and within the cytoplasmic vacuoles of the pneumocytes. Virions had an average diameter of 82 nanometers and a viral projection of 13 nanometers in length».
In this study, fibrin thrombi from small arterial vessels were observed in 33 of the 38 patients. «These findings could explain the severe hypoxemia that characterizes the clinical feature of ARDS in patients with SARS-CoV-2», adds the research.
The data collected «strongly supports the hypothesis proposed by recent clinical studies indicating that COVID-19 is related to coagulopathy and thrombosis».
For these reasons, «anticoagulants have recently been suggested as a potentially beneficial treatment in patients with severe COVID-19, although their efficacy and safety have not been demonstrated».

COVID-19 intensifies quadropathies and thrombi
The president of the Spanish Society of Thrombosis and Hemostasis (SETH), Jose A. Páramo Hernández, published an article in which he explains in detail how COVID-19 also affects everything related to the circulatory system, specifically blood.
«Sepsis is a complication of infectious diseases, especially bacterial, which is associated with an activation of coagulation, characterized by increased thrombin generation and a decrease in the body’s natural (anticoagulant) defenses. Thrombin is a coagulation enzyme that converts fibrinogen into fibrin, which is degraded by another defense system, called the fibrinolytic system, with the formation of a degradation product known as D-dimer «, explains Páramo.
The expert adds that in recent years the concept of immunothrombosis has been coined to describe the interaction between the immune system and the coagulation system as a response to infection by microorganisms, to prevent its spread.
«When these mechanisms are indiscriminately activated, as a consequence of a systemic infection, a condition called disseminated intravascular coagulation (DIC) occurs, characterized by the presence of massive deposits of fibrin in the circulation, which leads to organic damage and worsens the prognosis of the patients».
Various studies have demonstrated a link between the severity of coagulopathy, organ dysfunction, and mortality in patients with sepsis. In this sense – says Páramo Hernández – the current pandemic caused by the coronavirus COVID-19 represents a good example of viral infection associated with a systemic inflammatory response and activation of coagulation in symptomatic patients.
“Although, as previously mentioned, DIC is a recognized complication of bacterial infections, coronavirus infection can also cause it and condition thrombotic phenomena in various territories. For example, episodes of ischemia in the fingers of the lower extremities that can cause gangrene have been described», explains the doctor.
In this regard, he adds that «very recent results obtained from patients in the Wuhan area have shown that D-dimer, a marker of thrombin generation and fibrinolysis, constitutes a relevant prognostic index of mortality. These studies indicate that D-dimer levels higher than 1000ng / mL are associated with an 18-fold higher risk of mortality, to the point that they are currently included in the screening of all symptomatic COVID-19 positive patients».
«The fact that a coagulopathy is present in these patients has promoted antithrombotic strategies, especially in patients who enter the ICU and / or show organ damage or ischemic episodes, as previously described», said Hernández.
The head of SETH also indicates that “although the best antithrombotic strategy has not yet been established, it seems that low-molecular-weight heparins at prophylactic or intermediate doses should be indicated in these patients after admission to the ICU or when dimer values D are 4 times higher than normal, with therapeutic anticoagulation being reserved for cases in which a clear local or systemic thrombotic pathology is observed».
“The role of other strategies such as the use of antithrombin concentrates (only when their levels are below 50%) or thrombomodulin (not marketed in Spain) for the treatment of DIC continues to be controversial. In summary, properly selecting the candidate patient for antithrombotic therapy is essential to improve prognosis and reduce COVID-19 related mortality”.